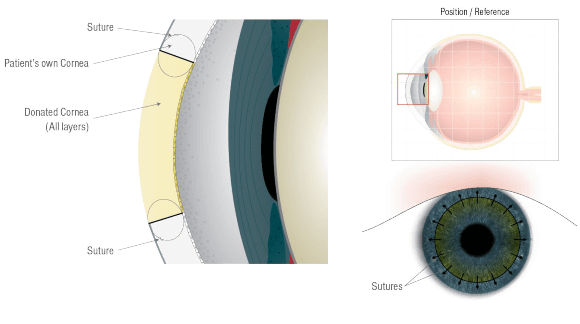
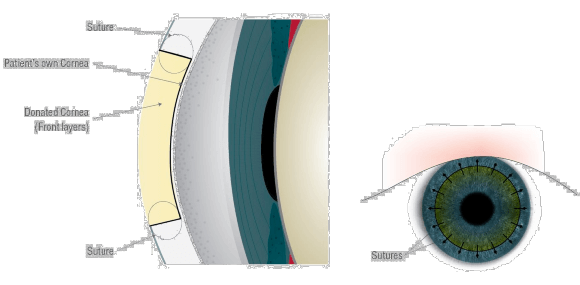
Corneal transplantation is a procedure where an abnormal shape (such as keratoconus) or poorly functioning scarred or opaque cornea is replaced with a donor cornea. Traditionally, all three layers of the cornea are replaced with a corneal transplant. Newer techniques allow selective replacement of the affected layers. This allows the patient to keep their own functioning layers. The three types of cornea transplant are penetrating (where all layers of the cornea are replaced), anterior (where only the front layers are replaced) and posterior (where only the back layer is replaced).
Corneal replacement, in full or in part, is sometimes warranted.
In this section
Surgery Information
Frequently Asked Questions
View all FAQsWhat is the Cornea?
The cornea (the “window of the eye”) is a clear, curved transparent structure at the front of the eye.
Where does the donated Cornea come from?
The cornea has been provided by a volunteer donor who has passed away and given permission for its use. Both the donated cornea and patient donating the cornea undergo intensive assessments. The donated cornea itself is examined to ensure that it is clear, examined under high magnification to ensure that the endothelial cell count is of adequate density and further tested to ensure that it is free of infection. An assessment is also made of the donor patient to ensure they have no evidence of significant infection or other pertinent illness. Modern techniques allow the cornea to be kept healthy for up to four weeks before transplantation.
News And Resources For Optometrists And Medical Practitioners